Positive publication bias in cancer screening trials
There are cases where major cancer screenings damage people’s health, but these cases are only rarely featured in the scientific evaluation of the screening programmes, according to a new literature review.
It is difficult for citizens and decision makers to know for sure whether it’s a good idea to introduce national cancer screenings for e.g. bowel or breast cancer.
So argues Bruno Heleno, GP, who is a visiting scholar at the Research Unit for General Practice, Copenhagen University, Denmark.
Together with colleagues, he has reviewed a series of studies that investigate the consequences of cancer screenings. They found that the studies usually report on the positive aspects of the screenings, but often avoid mentioning the negative aspects.
”It is important to know how much harm would be involved if society were to introduce a screening programme. It is therefore not enough that the scientific articles only mention the positive aspects of screening,” he says.

“There is a risk that doctors are spending too many resources on over-diagnosing and over-treating a great number of patients.”
Not all screenings are good
Screening a country’s citizens for e.g. bowel, cervical or breast cancer is not always a positive thing.
One reason for this is that screenings can detect precancerous lesions that will never cause the affected patients to become ill.
This, argues Heleno, creates a risk that doctors cause unnecessary concern and pain for patients by giving them a diagnosis and treatment.
It is important to know how much harm would be involved if society were to introduce a screening programme. It is therefore not enough that the scientific articles only mention the positive aspects of screening. There is a risk that doctors are spending too many resources on over-diagnosing and over-treating a great number of patients.
”The most common adverse effects are over-diagnosis and cases of false alarm. These harmful effects were only quantified in 7 and 4 percent, respectively, of the 57 cancer screening trials we have reviewed.”
Physical and psychological consequences
Health politicians use research findings to guide them in deciding whether to introduce a cancer screening programme; however, the new study reveals that the research provides an incomplete picture of the consequences of the screenings.
Heleno and his colleagues reviewed the scientific data from 57 studies, which investigated whether various screening programmes for cancer reduce the incidence of cancer and/or whether they prevent cancer deaths and deaths in general.
The studies reported on the positive results from the screenings. However, when looking at whether the studies accounted for certain negative consequences, Heleno and colleagues found that only few of them mentioned any of these.
We tried to get all the percentages as high as we could. Our only criterion was that the authors should clearly state the parameter and a number. So we could regard these figures as ‘worst case scenarios’.
The negative consequences of a cancer screening include:
- False alarm: doctors tell a patient that he or she is ill, without this actually being the case. Such cases were only mentioned in 4 percent of all the 57 studies. For those studies that only dealt with data from screened patients – i.e. where there was no control group – the figure went all the way up to 32 percent.
- Over-diagnosis: doctors detect a disease that would never have affected the patient’s life. Here, the figure was 7 percent.
- Negative psychological consequences: patients experience unpleasant psychological after-effects from the screening. These effects were only quantified in 9 percent of the studies.
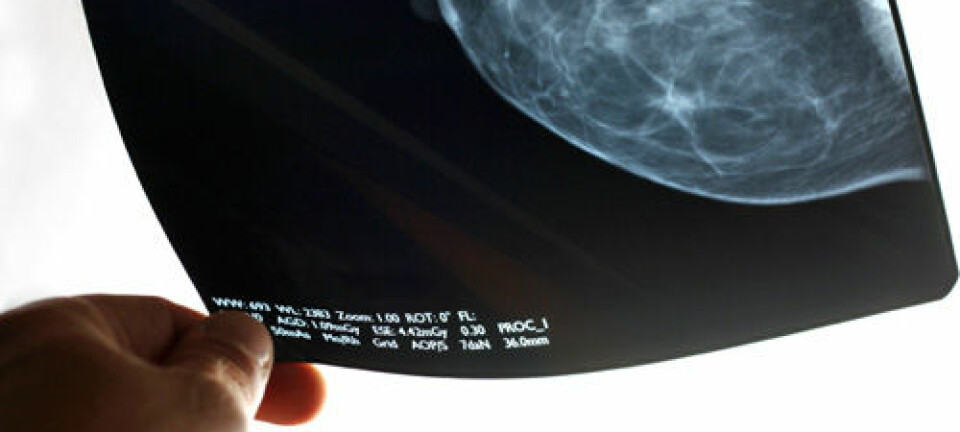
- Physical complications: patients feel pain during e.g. a mammography screening, or doctors take a sample that causes bleeding or a need for surgery. Here, the figure was 19 percent.
In comparison, 82 percent of the studies accounted for how many patients survived not only the duration of the test screenings, but typically a further 5-20 years.
”We tried to get all the percentages as high as we could. Our only criterion was that the authors should clearly state the parameter and a number. So we could regard these figures as ‘worst case scenarios’.”
Why the positive bias?
Nobody can say exactly why researchers tend to focus more on the positive aspects of the screenings:
”But from other people’s research I know that there are many possible explanations,” says Heleno.
Nobody can say exactly why scientists tend to focus more on the positive than the negative aspects of the screenings.
"But from other researchers’ work, I know that there are several possible explanations," says Bruno Heleno, and lists a few:
- Researchers are very enthusiastic about the good things that their research can lead to, and this creates a risk that they may put a particular focus on the positive aspects of a new drug or a new form of screening.
- In medical research in particular, significant economic and prestige-related interests may be involved. This may cause researchers to leave out the negative aspects of their research. This may also apply to screening research.
- Most screening tests were introduced in the ‘70s and the ‘80s. But it wasn’t until the ‘00s that researchers generally started to relate to the negative aspects of the screening programmes. It has therefore not been natural for researchers to consider the negative aspects. Heleno cannot, however, say whether a change in mentality is underway so that will change this picture in the coming years.
“We need new guidelines for screenings”
Despite criticism of his new literature review, Heleno has a clear stance:
“Researchers, research foundations and ethical boards need to sit down and agree on the guidelines for how the harmful effects in the studies of cancer screenings should be reported,” he says.
”Otherwise, neither decision makers, patients nor researchers can gain a clear picture of the pros and cons. They will also not be able to compare different screening methods. This is a complicated field and it is not easy to make a rational decision if it cannot be based on comparisons.”
------------------------
Read the Danish version of this article at videnskab.dk