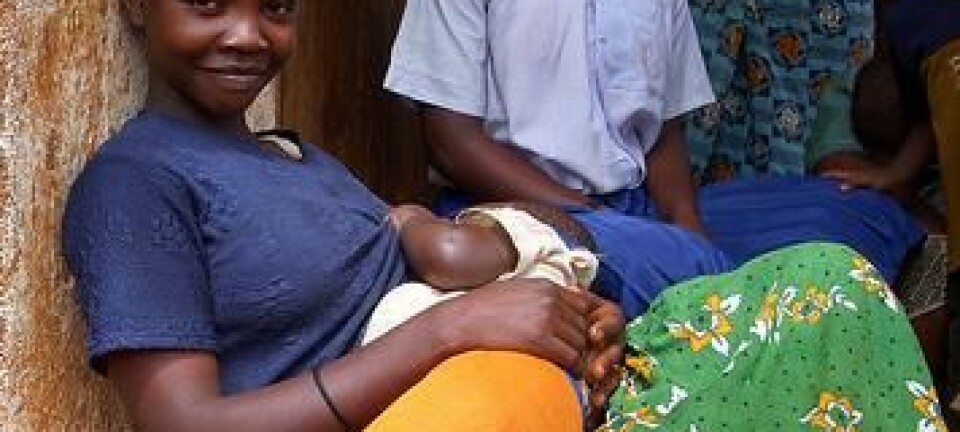
Women with breast infections stop breastfeeding
New mothers are more likely to stop breastfeeding in the first month after birth if they get an infection, says new study.
When a woman gives birth, her breasts suddenly take on a completely new role – they transform into vitalising milk cans for a tiny baby.
Unfortunately, this transition isn’t always smooth, and then infections can arise.
Women can also get infection in other parts of their body, such as the abdomen or the airways.
Many women stop breastfeeding as a result of these infections, and that can have serious health consequences for both mother and child, increasing the risk of e.g. cancer and obesity.

A new study conducted by the Department of Gynecology and Obstetrics, Horsens Hospital, Denmark, looked at the relationship between infections and breastfeeding, and counted how many mothers stop breastfeeding.
The study is published in the medical journal Acta Obstetricia et Gynecologica Scandinavica.
One in four gets infections after giving birth
Some 1,872 women who gave birth at Horsens Hospital in a year filled in a questionnaire, with 87 percent of them replying.
It turned out that almost one in four of the women experience some form of infection in the first month after birth.

A third of these infections are mild and do not require medical treatment, while the rest might require it, usually in the form of antibiotics.
The most frequent infections after childbirth are:
Breast infection (Mastitis) – 12 percent
Urinary tract infection – 3 percent
Breastfed children have fewer infectious diseases, better visual development, and in the long term they have lower blood pressure, lower cholesterol levels and a reduced risk of developing diabetes and certain intestinal diseases.
Vaginal infections (Vaginitis) – 3 percent
Sores – 3 percent
Respiratory tract infection – 3 percent
”By combining the survey answers with medical records, we could see a clear correlation between infections and cessation of breastfeeding,” says Peder Ahnfeldt-Mollerup, MD, a PhD student at the Research Unit of General Practice, University of Southern Denmark, who was one of the researchers in the study.
This, he says, was most evident in women with breast infections, sores and urinary tract infections.
“We have found a causal link between breastfeeding cessation and infection. But more thorough analysis is required to determine whether it’s actually the infection that causes the women to stop breastfeeding.”
Baby’s sucking can cause infection
Many factors play a part in when infections arise after childbirth. The production of milk, for example, may cause infections because the milk simply accumulates in the breast.
”The breast suddenly takes on a new function, one that it’s never had before. The milk ducts can for instance be constricted, and that can cause an infection,” says Ahnfeldt-Mollerup.
When the milk accumulates, this can mean that the number of naturally occurring bacteria increases.
The physical stress from breastfeeding, i.e. the baby’s suction, can also cause sores on the nipple.
Many reasons why women stop breastfeeding
Women who get these infections usually have less energy and are tired, and with breast infections in particular, the women feel pain and discomfort which only gets worse when they breastfeed their baby.
Some women stop breastfeeding simply because doing so is painful. Others stop because there’s not much milk in the breasts, explains the researcher.
“In principle, it could also be a fear of transmitting bacteria that keeps women from breastfeeding, but there have only been rare cases of this being an issue.”
These very rare cases are situations in which the infection develops into a boil formation where purulent matter enters the milk. In such cases it is advisable to extract all the milk and throw it away. If you’re not sure if you can breastfeed your baby, it’s a good idea to ask your doctor or health care provider.
“Some also stop breastfeeding because they’re taking antibiotics for the infection, but that’s not the right thing to do either. Most types of antibiotics are harmless to the child,” he says, adding that it’s important that mothers inform their doctor that they’re breastfeeding when they call in about an infection.
Mother’s milk is important
The World Health Organization recommends exclusive breastfeeding up to six months of age, and continued breastfeeding along with appropriate complementary foods up to two years of age or beyond.
If the breastfeeding stops within the first month after birth, it can have far-reaching consequences.
”Breastfeeding has a number of positive health effects for mother and child, both in the short and the long term,” says the doctor.
“Breastfed children have fewer infectious diseases, better visual development, and in the long term they have lower blood pressure, lower cholesterol levels and a reduced risk of developing diabetes and certain intestinal diseases.”
Furthermore, he adds, there’s a reduced risk of developing obesity in infancy, and there are indications that breastfeeding increases children’s intelligence. Breastfeeding in the first nine months reduces the risk of allergy and infantile eczema in children who are predisposed to allergies.
Breastfeeding can also reduce a mother’s risk of breast cancer and possibly ovarian cancer and type 2 diabetes too.
Important to get a good start with the breastfeeding
It’s recommended that women continue breastfeeding despite the infection. This actually speeds up the recovery from the infection, while at the same time providing the baby with the right nutrition.
The doctor mentions some useful techniques for avoiding infections:
“There’s a variety of ways to get the milk to flow to the breast, but what’s most important for a good start to breastfeeding is calm, patience and a good technique. Here you can get help from midwives and health visitors,” says Ahnfeldt-Mollerup.
“If you experience pain as a result of breastfeeding, it can sometimes be a good idea to use painkillers. If you have an infection while breastfeeding and you’re not sure how to go about with your breastfeeding, you can always contact your doctor or your health visitor.”
----------------------------------------
Read the Danish version of this article at videnskab.dk
Translated by: Dann Vinther