
New app could save you a trip to the hospital
Apps have great potential in the health service sector, but what are the challenges of implementing them?
Have you ever thought to yourself when leaving a consultation either with your GP or at the hospital, “was that it?”
After all the hassle of arranging time off work, finding a babysitter for the kids, perhaps a long journey and a struggle to find parking: Was it really worth all the trouble?
Patients with chronic diseases know this all too well. This is one of the reasons, the health sector is seeking technologies to support telemedicine sessions for patients and make virtual consultations a reality.
That is why CoLab Odense, in collaboration with the Department of Nephrology at Odense University Hospital, OUH, in Denmark, has provided patients with chronic kidney disorders the opportunity to measure their blood pressure at home and send their results directly to the physician at the hospital using a new phone app.
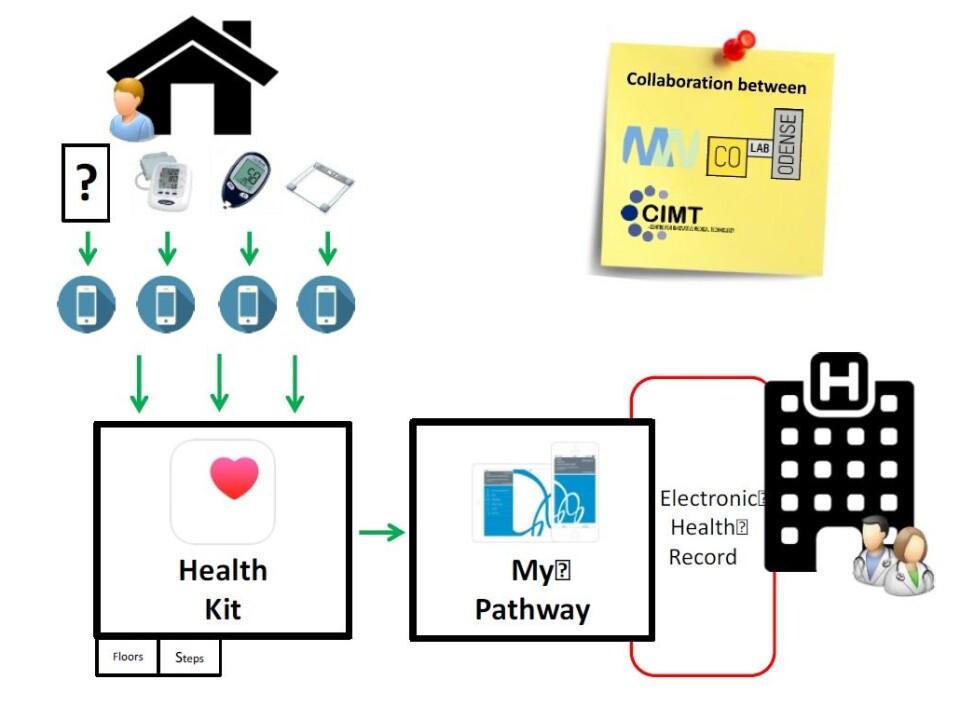
This makes it easy to replace outpatient visits with the use of Health Kit--a platform for data collection, which is already available as standard on new iPhones.
Health Kit works by receiving data from the blood pressure app, which in turn receives data from a blood pressure monitor via Bluetooth.
Read More: Birth control app invented by physicists gets EU approval
Blood pressure sent to the hospital with a single tap
All we had to do was connect Health Kit to My Patient Pathway--an app that allows patients to communicate with hospitals in the Region of Southern Denmark from the comfort of their own home.
The app sends data from the patient's phone directly to the hospital, as illustrated below.
As part of the project, patients were issued an iPhone and a blood pressure monitor. With them, they can measure their blood pressure and send it to the hospital with a single tap on the phone.
But in producing this system, we began to ask: How does consumer technology fit with health care services?
Read More: App will improve patient-doctor communication
Consumer behaviour and the patient of 2017
The hallmark of a consumer device, like a smartphone, is that it is targeted to the consumer, the individual, and not businesses, companies, or, for that matter, the hospital. The aim of the design of the device is that individuals get the most benefit from using it and the greatest possible freedom.
After all, mobile phone were originally designed for making calls, but today we use them to send texts, search for information (Google), find directions, play music, and now also as a health device.
Technology is an integral part of most people's daily lives. We use consumer devices in the form of tablets, smartphones, and pedometers and according to Statistics Denmark, the national statistics bureau, four out of five people aged 16 to 89 used a mobile phone to access the Internet in 2016.
But what happens when the consumer device becomes a part of the patient's course of treatment?
Read More: Smartphone app can reveal eye disease
Patients find the technology easy to use
We know from several studies that patients are ready to use technology both in the form of video calls and chat via an app, and that they find the technology easy to use.
New technologies need to be introduced, but quickly become easy to use once they are part of the patients’ everyday life.
This project is an example of how the human-technology-interface makes it easier for patients to perform the procedure themselves and simplify the procedure in general.
The app made the procedure easier for patients and consequently they were more likely to test their blood pressure on a regular basis.
Read More: App calms ADHD children before bedtime
It all depends on the interface
Patients may also find that such consumer devices empower them and improve their health, as previous research has shown.
Another plus is that the technology allows patients to stay at home during treatment or follow-up phase of treatment.
And it allows them to organise their time as they can independently measure their own blood pressure at a time that suits them. The same is true for the doctor, who looks at the results.
Read More: A wristband and an app for a better back
Is consumer technology compatible with the health care sector?
But is it really that easy to replace outpatient visits with a smartphone?
It almost sounds too good to be true. And in a way it is. There are many obstacles to overcome before smartphones can become an integrated part of the health care system.
Implementing My Patient Pathway has required quite a few detours:
1. Validated blood pressure monitor
The first problem was the requirement that the blood pressure monitor used, must provide valid measurements. This is not the case for all blood pressure monitors on the market, and identifying the validated blood pressure monitors requires close cooperation with clinical specialists.
2. Security requirements
Another requirement of the blood pressure monitor was that it had to be able to send data via Bluetooth to the smartphone. Equally important is whether the data measured by the patient will be shared in the cloud.
This is still a challenge, as some blood pressure measuring apps require that the user creates an account with the company in question and sends the records to them. It is of course up to the individual if they wish to create such an account, but as a public authority, we are not allowed to encourage patients to share their data with a 3rd party.
Our app complies with the security requirements, if the app that measures the blood pressure does not require the user to create an account.
3. The grandchild's blood pressure
To ensure that it is the patient’s and not the grandchild's blood pressure that ends up in the patient records, the patient must sign the data in My Patient Pathway, before it is transmitted to the hospital.
4. When can I expect an answer?
Due to our texting and snapchat culture, we expect quick responses – and find it difficult to understand when the response is delayed. It is too cost-intensive for a clinician to keep an active eye on the submitted blood pressure data as it is registered. It is therefore important to agree with the patient and/or community nurse, when they can expect their data to be analysed.
Read More: Soccer is as effective as blood pressure drugs
Technology on collision course with legislation
To achieve the shortcuts that technology offers may take some time yet, since it often collides with restrictive legislation for sharing sensitive, personal data.
Another restriction is that there are currently only a few devices that can be used in the health care service, because most apps require you to submit your personal data to the app. The question is, if the companies’ business models will allow them to compromise with regards to the data that can be generated by these health apps, and allow a greater consumer choice of devices for people wishing to use such services?
Further more, patients are moving at a faster pace than both the health sector and the law due to their daily use of the technology. For example, it is tempting to begin using texts, messenger, or facetime to contact health professionals but the law does not yet allow this.
Paradoxically, the law that protects patient data also ends up obstructing exactly the quickness and agility that comes with technologically mediated contact. And in the worst-case scenario is that such technology remains an untapped potential.
Consumer devices are adapted to the needs and usage of the users and legislation should be adjusted correspondingly. Such flexibility is necessary to allow both citizens and socio-economics to benefit from the technological solutions that the health care sector is on the brink of being able to implement.
This requires new legislation, but it also requires companies to find a business model that prevents apps having automatic access to patient data.
---------------
Read this article in Danish on ForskerZonen, part of Videnskab.dk






.gif)


